By: Dr. Brian P. Kinmartin, PT, DPT, MTC, OCS, STC, CWcHP, Cert. DN
One of the most common causes of foot pain that affects roughly two million Americans a year and 10% of the population during their lifetime is known as plantar fasciitis. Plantar fasciitis is a painful inflammatory condition of the thick band of tissue (fascia) on the bottom of the foot which runs across the bottom of the foot and connects your heel bone to your toes. Under normal circumstances, the plantar fascia acts like a shock-absorber on the bottom of the foot with walking and weight bearing activities. When standing up and putting weight down through your foot the plantar fascia stretches and absorbs the stress or energy of the body supporting the arch in the foot. Like all tissues, if the tension becomes too great or occurs too often, it can create small tears in the fascia. Repetitive tearing can cause the fascia to become chronically irritated or inflamed, resulting in plantar fasciitis.
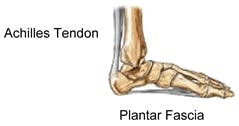
Plantar fasciitis is most common between the ages of 40 and 60, it seems to occur more often in women than men, it is more likely to occur in people who are obese or who have a high body mass index, and it is more prevalent in people who perform activities that place a lot of stress on the heel bone and the attached tissues, such as runners and people with occupations that require a lot of walking or standing on hard surfaces, such as factory workers, teachers and waitresses. People who have faulty foot mechanics also are predisposed to suffering from plantar fasciitis. If you are flat-footed, or have a high arch or even just have an abnormal walking pattern, it can unevenly distribute your body weight when you are up on your feet, putting added stress on the plantar fascia making you more susceptible to injury. Improper shoe wear is another factor that can make you more susceptible to plantar fasciitis.Shoes that are thin soled and have poor arch support lack the ability to absorb shock when on your feet, if wearing shoes with high heels, the achilles tendon or the thick tendon attached to the back of the heel can shorten, causing strain on the tissue around the heel, which includes the plantar fascia.
The symptoms of plantar fasciitis include foot pain that usually develops gradually; it usually affects just one foot, although it can occur in both feet simultaneously. It usually is worst with the first few steps in the morning after waking, and can be triggered by long periods of standing. Another symptom of plantar fasciitis is decreased ankle dorsiflexion, or a decreased ability to lift the foot bringing your toes up towards your head. This can be due to a tight achilles tendon which attaches to the heel bone. A tight achilles tendon pulls the foot downwards towards the floor making it tough to lift the foot the opposite way. This can cause excessive stress to the plantar fascia, resulting in chronic injury and inflammation.
Upon a diagnosis of plantar fasciitis your physician may recommend several different forms of treatment. Nonsteroidal anti-inflammatory drugs (NSAIDs) may be recommended to assist with pain and inflammation. Corticosteroids may be used through two different delivery processes, iontophoresis in which a corticosteroid solution is applied to the skin over the painful area and the medication is delivered with the aid of an electric current transdermally, or a corticosteroid may be injected directly into the plantar fascia by your physician. Night splints may be recommended to hold the plantar fascia and achilles tendon in a lengthened position overnight so that it can be stretched more effectively. Orthotics may also be recommended by your physician to help distribute pressure more equally in your feet with standing and walking activities.
Another form of treatment recommended by your physician may include a referral to physical therapy. Physical Therapists are skilled medical practitioners trained in biomechanics and human anatomy. At your initial consultation the Physical Therapist will perform a mechanical examination of your foot and ankle attempting to determine the exact cause of the irritant to the plantar fascia. Modalities such as ultrasound may be used to break up scar tissue, promote healing, and increase blood flow in the area. Soft tissue mobilization may be used to help reduce muscular tightness and tension in the plantar fascia. Iontophoresis may also be used as discussed to assist with decreasing swelling and inflammation. A Physical Therapist will also instruct you in a series of exercises and stretches to the plantar fascia and achilles tendon in order to improve ankle and foot alignment, mobility and to strengthen the lower leg muscles. A therapist may also use athletic taping techniques to temporarily support the bottom of your foot, limiting stress to the plantar fascia and allow healing.
Brian P. Kinmartin, PT, DPT, MTC, OCS, STC, CWcHP, Cert. DN, owner of Professional Rehabilitation Services in Pawleys Island and Myrtle Beach, South Carolina has earned his Doctorate degree in Physical Therapy, is board certified in Orthopedics, is a Certified Manual Therapist trained inmanipulation of the spine, pelvis and extremities, and is also a certified vestibular therapist. For further information on this topic or questions about obtaining a referral or making an appointment at Professional Rehab, please contact Brian P.Kinmartin PT, PT, DPT, MTC, OCS, STC, CWcHP, Cert. DN at our Pawleys Island office at 843-235-0200, Richard A. Owens, PT, MS, OCS, Cert. SHT, CWcHP, Cert DN at our Myrtle Beach office at (843) 831-0163 or Richard DeFalco, DPT, OCS, CSCS, CWcHP, Cert. DN at our Myrtle Beach office at (843) 839-1300, or visit our website at www.prsrehabservices.com
